How Vicarious Liability Affects Dental Practice
Case Study
Marc Leffler, DDS, Esq.
January 16, 2025
Reading time: 7 minutes
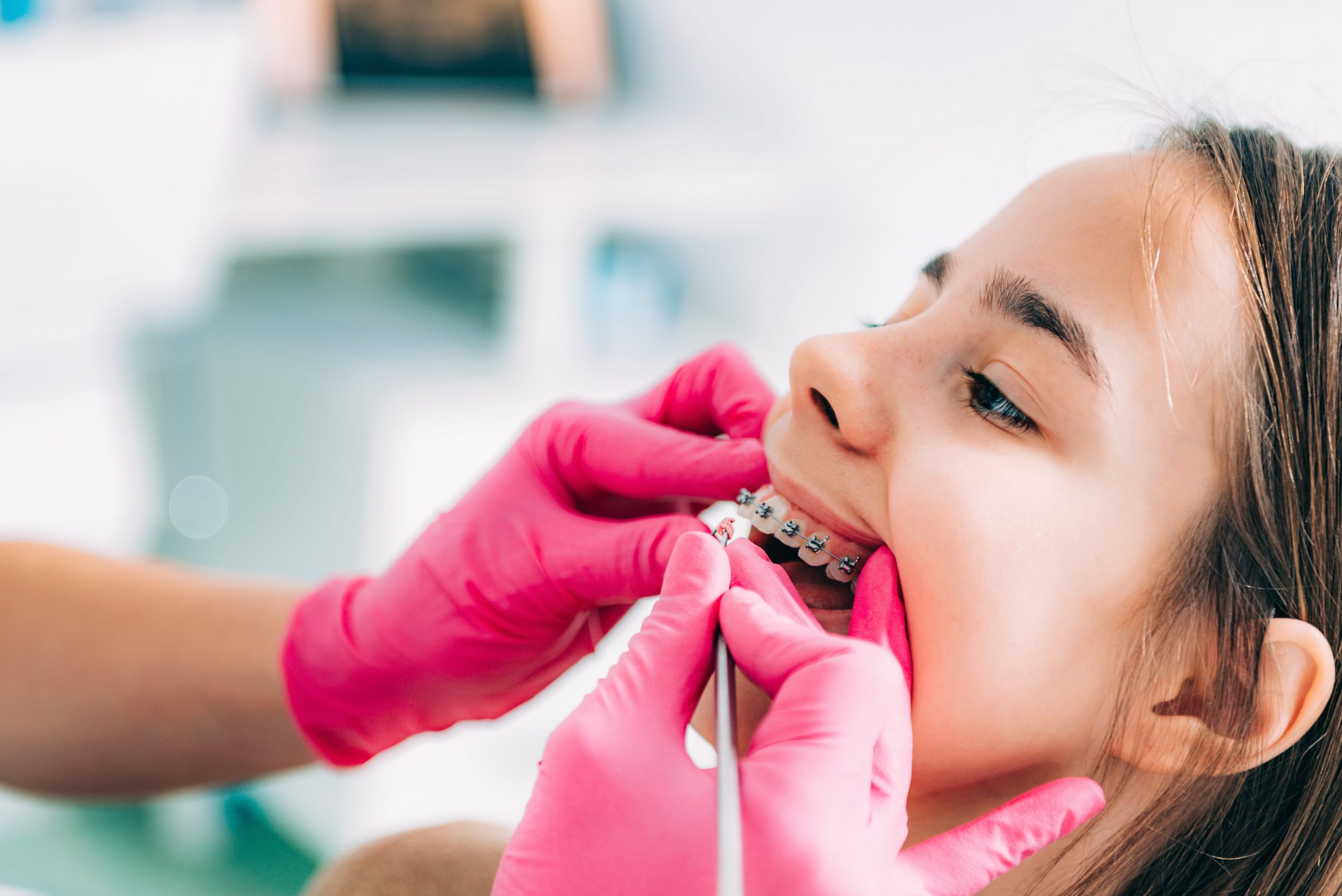
Under state dental regulations, only licensed professionals can treat patients, with the supervising dentist held responsible through vicarious liability. In this case study, an orthodontist faces liability after an “untrained” dental assistant drops a bracket into a patient’s mouth.
Key Concepts
- Vicarious liability for dentists
- State Dental Practice Acts
- Staff management and communication
Background Facts
Dr. D had a very busy orthodontics practice, and like most other offices, the after-school time slots were particularly hectic. Ms. K was a dental assistant who had worked with Dr. D for many years, having learned her competency from him directly, “on the job”. On a typical day for the office, T, a 16-year-old girl presented for treatment. She required the replacement of 3 orthodontic brackets, which were to be bonded into place. As was her regular activity, Ms. K seated T, draped her, and prepared to bond the needed brackets into place. Dr. D worked from room to room, performing treatments that needed his direct care.
In the process of bonding 1 of the brackets, Ms. K lost control and dropped it, falling into the back of T’s mouth and out of sight. T did not even realize what had happened. At the end of the visit, with all planned brackets bonded on, Ms. K mentioned to Dr. D that a bracket had fallen and was not retrieved. Dr. D explained to T and her father exactly what took place, and told them that there was no way to know if it fell into a lung, into the esophagus, or possibly even came out of the mouth harmlessly. He suggested that T have a medical evaluation with radiographs to determine its location.
T and her father went to a free-standing medical office nearby, where imaging was performed. The bracket was located in the stomach, according to the reading of an off-site radiologist. Because of its tiny size and shape, the physician treating T saw no reason to have an endoscopy performed, instead opting to allow it to pass with feces. The physician instructed T as to how to examine her feces for several days; T did exactly what was asked of her, and was able to find the bracket 2 days later. She had no medical complications.
Nearly 6 weeks later, T’s father received a bill for the off-site radiologist, who was located in a different State. T was covered by a medical insurance plan which only paid providers who practiced in her State of residence and its 3 adjoining States, neither of which was the radiologist’s location. T’s father contacted Dr. D and asked that he pay for the radiologist’s fee. Dr. D said that he saw no obligation to do so, arguing that he cannot be responsible for the limitations of the family’s medical plan. T’s parents were divorced, but her mother was told about all of the events; while T’s father was angry about how Dr. D handled the issue, the mother was not, so she stepped in to accompany T to all further orthodontic appointments until treatment was uneventfully completed.
Legal Action
T’s father reached out to several attorneys who advertised as “dental malpractice lawyers”, but none would take on a case because there were no physical injuries and because the monetary damages in the way of radiology fees were too small to make a case financially worthwhile. But one of the attorneys suggested that T’s father could file a Dental Board complaint, which is exactly what he did.
Upon receiving from the Board a request for records and an explanation of the events, Dr. D contacted his malpractice insurance carrier to seek advice. Pursuant to his policy, Dr. D was entitled to have an attorney assigned to his matter. The attorney responded to the Board with a copy of the chart and a statement that directed the Board to the chart entry which documented the events.
Soon after, the Board notified the attorney that its investigator wished to conduct taped interviews of Dr. D and Ms. K. They complied. Ms. K was interviewed first, and she explained the events, just as they occurred. The investigator then asked Ms. K about her educational background, which ended upon her high school graduation; after working in the retail clothing business for a few years, she joined Dr. D’s practice, where he taught her the various tasks that he wanted her to perform as an orthodontics assistant, and watched over her directly until she gained experience and competence.
During Dr. D’s interview, he was questioned as to why he permitted Ms. K to perform what the Board viewed as dental treatment, allowed in that State to be undertaken only by a dentist, a dental hygienist, or a certified dental assistant. Dr. D declined to respond to that question, based upon the advice of his attorney in advance of the interview, with the knowledge that such a non-response would likely lead to some sanction against his dental license, but probably nothing more. The Board followed with 2 letters, 1 to Dr. D and 1 to Ms. K. Dr. D was advised that he was in violation of the State’s Dental Practice Act by permitting an untrained person to perform dental treatment, and forced to pay a substantial fine, with a stayed suspension from practice of 6 months, which would not be enforced unless he further violated the Act; if he chose to oppose the findings, and seek a full Board review process, he could be, according to his attorney, subject to more severe penalties. He opted to accept the terms. Ms. K’s letter advised her that she was in violation of the law by practicing dentistry without a license, but that no referrals outside of the Board would be made so long as she ceased any further unlawful acts in that or any other dental practice.
Takeaways
By way of a concept known as vicarious liability, a dentist (and/or a dental entity) is responsible for the acts of those who work under the dentist’s supervision, whether that supervision is direct or simply implied. Therefore, even though Dr. D did not perform any care upon T on the day she swallowed the bracket, had an attorney opted to take on a case of dental malpractice, or had T’s father chosen to proceed with a lawsuit on his own (pro se), Dr. D would have been legally responsible for any negligent acts on the part of Ms. K. It is important for dentists to be aware of this in the course of overseeing the actions of all of their staff members that are involved with patient contact to any degree. And it is critical that they be aware of which duties may be properly delegated and which must not.
This case also demonstrates the importance of dentists knowing, and following, the rules set forth in their State’s Dental Practice Act. That is not to say that dentists need to understand the nuts and bolts of all of the legalities within the Act, but it does mean that dentists need to follow the Act’s contents as a reasonable dentist would. Generally, Practice Acts are written in language that is readily understandable to those without a legal background, so it is a good idea to become familiar enough with the terms to be able to be in compliance. And if there is something in the Act that a dentist might not fully appreciate, the Dental Board might serve as a source for information, and if not, contacting the malpractice insurance carrier for input, instead of or prior to asking an attorney, is often helpful.
Addressing some clinical issues, it is far from uncommon for small dental instruments and objects to be dropped from the working field into the back of the mouth and unable to be located. Swallowing or aspiration is almost always a preventable event, if appropriate precautions applicable to the particular situation are employed. But when it does occur, actions like Dr. D took in this case – referring the patient immediately for a medical evaluation, at a medical office or hospital – are proper and necessary. Until a dropped object is located as being in the respiratory tree, in the gastrointestinal tract, or not in the body at all, the next steps become mere guesswork, which is never a satisfactory approach. Based upon given situations, the time may well be of the essence for retrieval, so the sooner a dental procedure can safely be stopped and a referral made, the better off the patient will be.
Finally, a lawsuit averted is always a positive. But patients, and their representatives, have options beyond that, especially if they feel denied of any resolution. Here, had Dr. D agreed to pay the radiologist’s fee, there is a good chance – or at least a better chance – that no actions against him would ever have been taken. When faced with an option toward resolution, even if not particularly palatable, due consideration ought to be given in favor of what would be best, for all involved, before a stance is taken.
Note that this case presentation includes circumstances from several different closed cases, in order to demonstrate certain legal and risk management principles, and that identifying facts and personal characteristics were modified to protect identities. The content within is not the original work of MedPro Group but has been published with consent of the author. Nothing contained in this article should be construed as legal, medical, or dental advice. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your personal or business attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
Additional Risk Tips content
Why Accurate Documentation Matters Before Referral and Surgery
In this case study, inaccurate referral information leads to wrong site surgery and a malpractice claim. Read the case to learn how to prevent errors.

How to Stay Passionate in Your Dental Career
Insights on sustaining passion in a dental career through education, community support, work-life balance, and meaningful patient relationships.

Dentist’s Choice of Radiographic Technique Leads to Lawsuit
In this case study, radiographic imaging decisions for a dental implant procedure leads to a malpractice suit. Read the case to learn how the case unfolded.
This document does not constitute legal or medical advice and should not be construed as rules or establishing a standard of care. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
MedPro Group is the marketing name used to refer to the insurance operations of The Medical Protective Company, Princeton Insurance Company, PLICO, Inc. and MedPro RRG Risk Retention Group. All insurance products are underwritten and administered by these and other Berkshire Hathaway affiliates, including National Fire & Marine Insurance Company. Product availability is based upon business and/or regulatory approval and/or may differ among companies.
© MedPro Group Inc. All rights reserved.