Patient Sues Dentist After Refusing X-Rays
Case Study
Marc Leffler, DDS, Esq.
June 26, 2025
Reading time: 8 minutes
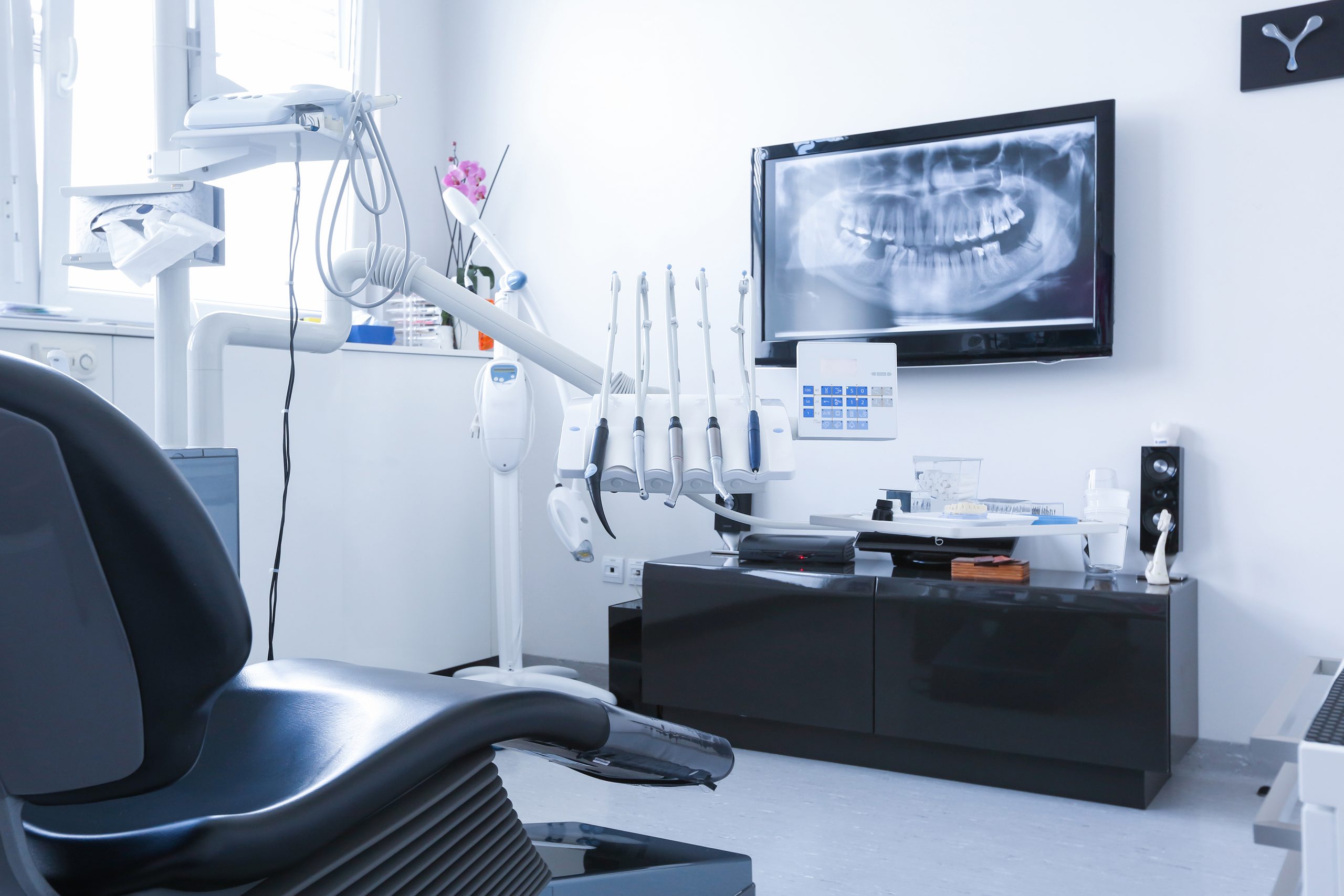
Patient refusal is an aspect of dental care dentists must navigate. In this case study, a patient presents to her dentist with tooth decay but refuses x-rays. The dentist unsuccessfully attempts to treat the decay without x-rays. Later, the patient sues the dentist for negligence.
Key Concepts
- Patient refusal in dental care
- Informed consent and refusal
- Dental standard of care
Underlying Facts
T, a 54-year-old woman, presented to her long-time general dentist, Dr. E, having not seen him for nearly 3 years, due in part to the COVID pandemic and in part to a “dislike” of going to the dentist. In the past, Dr. E had performed prophylaxis with spot deep scaling, as well as a number of 1- and 2-surface restorations. At the most recent prior visit, bitewings were taken, which were not concerning from the standpoint of decay. T’s oral hygiene had always left much to be desired, and her diet contained a good deal of sugary food and drink.
At the current visit, Dr. E performed a clinical examination. Several teeth had “explorer catches” on their occlusal surfaces, leading Dr. E to conclude that decay was present, at least occlusally, and he also saw indicators of potential interproximal decay. Dr. E explained that he needed to do a full-mouth series of radiographs, because it had been a number of years since they’d last been done, and to further assess the teeth of potential clinical concern. T said that she had been closely following a few online blogs which suggested that dental x-rays are damaging to the body and are not needed for dentists to make accurate diagnoses. Dr. E responded that he disagreed with those concepts, as did all of “mainstream dentistry.” He explained that there was no way to assess the condition of teeth by a clinical examination alone. But T persisted in her beliefs and insisted that Dr. E do whatever fillings he saw clinically fit.
Not wanting to leave obvious decay untreated, he relented and agreed to treat those teeth which he determined to be clinically decayed. With local anesthesia, he proceeded to excavate occlusal decay on teeth #s 19 and 20 and placed restorations in them. Dr. E then turned his attention to tooth #30. He found and removed a significant amount of occlusal decay which extended mesially and pulpally to the extent that it had invaded into the pulp chamber. When he explained to T that she would require root canal therapy, she became outwardly upset and demanded to know why she had not been advised of that prior to the start of treatment. Dr. E responded that T’s refusal to allow radiographs to be taken prevented him from knowing the extent of decay present. T eventually allowed the endodontic procedure to go forward, but when told that a post and crown would then be needed, she demanded that Dr. E perform those free of charge. He would not agree, so T left his care upon completion of the root canal therapy.
Nearly a year later, Dr. E received a call from a hospital dental resident who had admitted T for a severe infraorbital infection, secondary to a grossly decayed upper first molar. The resident explained that T advised her of recent treatment by Dr. E and wondered why that tooth had not been treated. Dr. E discussed the x-ray refusal, which heavily limited his diagnostic ability. T was treated with IV antibiotics and multiple I&Ds, remaining hospitalized for 4 days and incurring costs well above her insurance coverage.
Legal Action
Angered by those costs and her entire hospital experience, T retained an attorney to look into a potential dental malpractice suit against Dr. E. Once records were obtained, T explained to her attorney about the lower right tooth that started as a filling but ended up as a root canal, necessitating a post and crown which she could not afford. The attorney filed suit against Dr. E on behalf of T, asserting malpractice regarding his treatment of tooth #30 and his failure to diagnose decay on tooth #14 (thereby leading to the hospitalization and surgery). Following service of the legal papers, Dr. E advised his malpractice insurance company, which provided him with defense counsel.
In conjunction with filing an Answer, in which Dr. E formally denied all allegations, defense counsel filed a motion seeking summary judgment – essentially an early dismissal on the merits (or lack of merits) of the plaintiff’s case. Dr. E’s expert argued that Dr. E’s “hands were tied” by T’s refusal to allow any x-rays, thereby greatly limiting his ability to determine all that was going on in T’s mouth. In opposition to the motion, T’s counsel obtained an affidavit from an experienced dentist who would serve as an expert for T. The affidavit was to be included with the legal papers submitted to the judge in support of allowing the case to move forward. The thrust of T’s expert’s opinion was that Dr. E placed himself in a negligent position by acceding to the demands of his patient and proceeding with treatment that he acknowledged was based upon incomplete diagnostic information.
The judge denied Dr. E’s motion and allowed the case to move forward to be decided by a jury. Dr. E worked closely with his attorneys to weigh the strengths and weaknesses of T’s case and his own defense. In the end, Dr. E realized that, despite his best intentions, he had allowed his patient to dictate to him what he “must do,” rather than hold fast to principles he knew to be sound. Through negotiations, assisted by a court-appointed mediator, Dr. E consented to allow his carrier to pay, on his behalf, an amount of money which would, after attorney fees, reimburse T for her out-of-pocket hospital and medical expenses, but nothing more. T accepted that offer, resolving the case.
Takeaways
T fits into a category of a patient type sometimes referred to as “patient as dentist.” These patients, who tend to engage in litigation when the treatments they insisted upon do not turn out well for them, demand that their dentists go along with their dental treatment approaches. In effect, they are making decisions that are usually left to the discretion of the dentist. Patients have the absolute right to refuse any treatment they choose, but dentists ought not to allow a patient’s demand to carry the day. If a patient’s refusal places the dentist in the position that the dentist’s care (broadly viewed) would be compromised if carried out, then it is in neither the patient’s nor the dentist’s best interests to go forward with the demanded treatment.
Readers might reasonably stop at this point and rhetorically ask how this approach is not counter to the concept of informed consent, which contains the concept of advising patients of their options and then letting them decide which of those options they wish. The distinction lies in one word – “viable.” Obtaining a patient’s informed consent means allowing patient choices after advising them of the foreseeable risks, the benefits, and the viable options available. So, unless a patient like T were to insist upon an option that is dentally appropriate, that option is not viable, and therefore not one that falls within the bounds of informed consent. Here, the “option” that T created on her own – treating her caries without the benefit of radiographs – was not dentally appropriate, and therefore not viable, so it was not an option to have been exercised.
Dentists are ethically and legally bound to act toward their patients only in ways which fall within the standard of care, which is loosely defined as acting in ways that a reasonably prudent dentist would act under similar circumstances. While dentists will probably disagree as to how to interpret the components of that definition, it is fair to say that the vast majority of dentists would agree that this all boils down to doing what is in each patient’s best interests. And the vast majority of dentists will likely agree that – absent some rare, unusual circumstances – performing operative dentistry without having reviewed current radiographs first, is not in most patients’ best interests.
A thought process that likely passed through Dr. E’s mind was that, despite T’s refusal to allow x-rays, he was doing the patient a greater service than disservice by treating at least some of her decay. In that way, at least some teeth would be in a better state than if left untreated. Although arguably morally sound in concept, dental science generally does not subscribe to that reasoning, instead in favor of obtaining diagnostics before acting. That was the approach of T’s expert, and once hearing that, Dr. E realized that mainstream dentistry was not on the side of his compromise.
We conclude with a concept that is briefly and otherwise touched upon in this case study, namely the provision of dental services free of charge in order to calm down an upset patient. To start, that is a personal decision to be made in the face of very specific and individual people and events – there is no right or wrong. As with so many things in life, it involves a risk/reward analysis which is often far more subjective than objective. Dentists should consider that, at the time that such dentist-patient agreements are made, the patient is already dissatisfied and, depending upon personality, possibly thinking along litigious lines. So, when it comes to fee waivers, refunds, or the actual transfer of money to a patient, dentists can best protect themselves by engaging their malpractice carrier (or possibly a practice attorney) to make sure that any necessary paperwork is prepared and executed properly and to be certain that all state laws and regulations are fulfilled. The saying, “no good deed goes unpunished,” is best headed off prospectively.
Note that this case presentation includes circumstances from several different closed cases, in order to demonstrate certain legal and risk management principles, and that identifying facts and personal characteristics were modified to protect identities. The content within is not the original work of MedPro Group but has been published with consent of the author. Nothing contained in this article should be construed as legal, medical, or dental advice. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your personal or business attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
Additional Risk Tips content
Why Accurate Documentation Matters Before Referral and Surgery
In this case study, inaccurate referral information leads to wrong site surgery and a malpractice claim. Read the case to learn how to prevent errors.

How to Stay Passionate in Your Dental Career
Insights on sustaining passion in a dental career through education, community support, work-life balance, and meaningful patient relationships.

Dentist’s Choice of Radiographic Technique Leads to Lawsuit
In this case study, radiographic imaging decisions for a dental implant procedure leads to a malpractice suit. Read the case to learn how the case unfolded.
This document does not constitute legal or medical advice and should not be construed as rules or establishing a standard of care. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
MedPro Group is the marketing name used to refer to the insurance operations of The Medical Protective Company, Princeton Insurance Company, PLICO, Inc. and MedPro RRG Risk Retention Group. All insurance products are underwritten and administered by these and other Berkshire Hathaway affiliates, including National Fire & Marine Insurance Company. Product availability is based upon business and/or regulatory approval and/or may differ among companies.
© MedPro Group Inc. All rights reserved.