Sedation of High-Risk Patient Leads to Sanctions Against Dentist
Case Study
Marc Leffler, DDS, Esq.
January 16, 2025
Reading time: 7 minutes
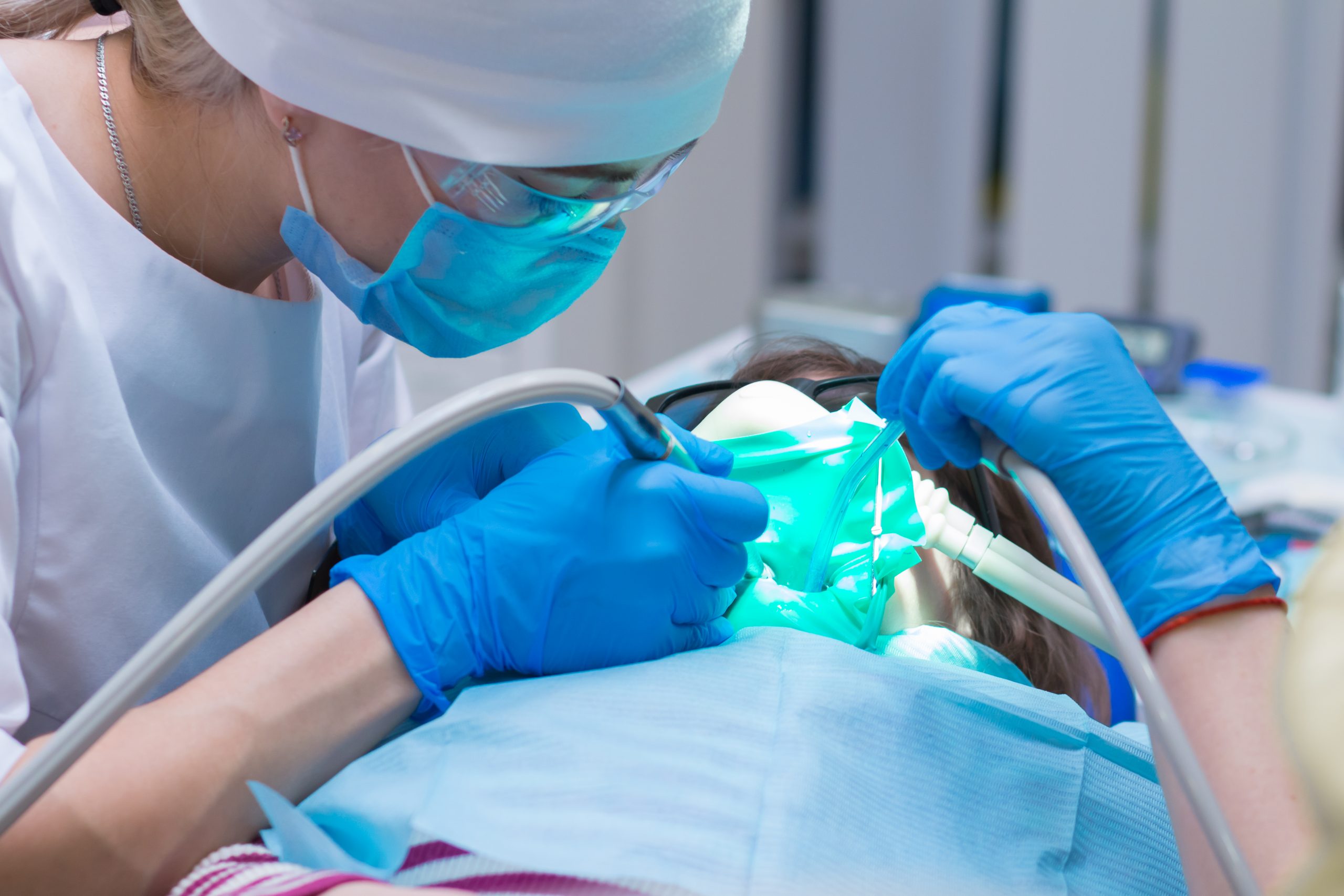
To make an informed decision about the safety of sedation for each patient, it is crucial for dentists to consider a patient’s medical history and all the possible complications that could occur when they are put under. In this case study, a dentist inappropriately sedates a high-risk patient, leading to sanctions.
Key Concepts
- Patient selection for sedation
- Risks associated with in-office sedation for dental procedures
- Patient safety
Background Facts
Dr. E was a general dentist, relatively new to practice in a suburb of a large city. In an effort to maximize what she could provide for her patients, she took a series of state-approved courses which, upon completion, permitted her to deliver moderate parenteral (non-GI) sedation to patients in her office. She diligently complied with the related requirements regarding having her office properly equipped with a “crash cart” and monitoring and assuring that all her chairside staff were CPR-trained.
H was a 68-year-old male patient who had been seeing Dr. E for a few years. He wore a double-distal-extension mandibular partial denture but was dissatisfied with its retention and function. Dr. E had spoken to him about placing bilateral posterior mandibular implants to serve as a basis for fixed prosthetics, but he resisted due to his anxieties about surgery unless he were “asleep.” After Dr. E obtained her qualification to deliver IV sedation, she offered that to H, and he agreed to have the implants placed in two separate appointments, each one focusing on placement on one side only.
Medically, H was obese, at 5’8″ tall and weighing 231 pounds (a BMI of 35.1), and he had COPD from years of smoking which he had since given up, and obstructive sleep apnea (OSA) for which he regularly used a CPAP machine. Dr. E sought and obtained medical clearance for the implant surgery under IV sedation from H’s primary care physician, so she felt confident in proceeding as planned.
On the date of surgery to place 3 implants in the left mandible, H was NPO for more than 8 hours and was accompanied by his adult son. Dr. E placed a nasal mask on H, providing a 60%/40% N2O/O2 flow; this was followed by the delivery of the first dose of Midazolam intravenously, which was supplemented and titrated as necessary over the next 2 ½ hours. Local anesthesia was injected after H became relaxed and somnolent. Monitors said to Dr. E that her patient was stable throughout. Upon completion of the procedure, H unsteadily walked to the office recovery area, assisted by both a dental assistant and H’s son. After approximately 30 minutes, H appeared as still being “out of it,” so Dr. E gave him a dose of Flumazenil to reverse the effects of the Midazolam. H steadily became more alert, so he was discharged home; H’s son took him home and stayed with his father for the rest of the day. About 4 hours later, H’s son noticed that his father seemed to be slipping backward into a sleepier state, and this process continued to the point that it became difficult to arouse him, with an irregular snoring pattern happening. The son contacted EMS; upon EMS arrival, H’s SpO2 (oxygen saturation) measured 81% and H’s depressed mental status and breathing pattern did not improve. With the approval of the ED physician, H was intubated and given supplemental oxygen while being transported to the hospital, where he remained for the next 8 days until he was able to breathe on his own and maintain an SpO2 of 94-96%. According to H, his son, and H’s friends, he was never able to return to the usual daily activities that he enjoyed prior to the implant procedure.
Legal Action
Although H’s son met with several attorneys on his father’s behalf, he was unable to find any who would proceed with a malpractice action against Dr. E, for the general reason that it would be difficult to objectively demonstrate compensable damages. But the son was very upset by what he saw in his father’s ability loss, so he filed a Board complaint against Dr. E.
Upon receipt of the complaint, Dr. E reached out to her malpractice carrier, following which counsel was assigned by the carrier to represent her before the Board. All records were provided in a timely manner to the Board, and Dr. E appeared, with her attorney, for several interviews before Board members and a dental anesthesiologist “expert.” Dr. E’s testimony relied heavily on the facts that she had obtained pre-sedation medical clearance from H’s physician, so she felt fully justified in her patient selection, and that she had kept H in her office until he was clearly in a state that was stable enough for discharge.
At the conclusion of its investigation, the Board issued a report in which it found a number of care deficiencies on the part of Dr. E and levied sanctions against her, namely a fine, a 2-month suspension from practice, and revocation of her sedation permit. The major findings of the Board, which it detailed in its report, were that Dr. E had inappropriately delivered in-office sedation to a patient who was not a suitable candidate and for whom she did not take proper precautions during the post-sedation period; the Board viewed the obtained medical clearance as essentially irrelevant to the issues, because the ultimate decisions about treatment ultimately lie with the treating practitioner.
Citing to an attached set of findings by the Board’s expert, the Board first determined that H had been misclassified by Dr. E as an ASA (American Society of Anesthesiologists) Class II patient, when he was actually a Class III; the Board pointed to the fact that the required coursework taken by Dr. E included a policy guideline that patients with greater than a Class II designation ought not to be sedated in an office setting unless a medical or dental anesthesiologist was present to manage the anesthesia aspects of care. The Board determined that, while H’s obesity status placed him as an ASA II, his OSA requiring CPAP use meant that this disease was “severe,” placing him as an ASA III, and his COPD, alone, categorized H as a Class III. All told, H was an ASA Class III, making him an inappropriate choice for in-office sedation under these circumstances, according to the Board. Furthermore, the Board found that Dr. E had failed to consider and take into account the relative half-lives of the drugs she employed, Midazolam and Flumazenil. The Board’s expert detailed that Midazolam’s half-life was measured on the order of 1.5-2.5 hours, while its reversal agent, Flumazenil, had a half-life of approximately 30 minutes; so, estimating that 4-5 half-lives are necessary for “clinical elimination,” Dr. E failed to take into account that the sedative agent would stay in H’s system for far longer than its reversal agent, leading to a revived level of sedation – with decreased respiration – once the reversal drug had effectively dissipated.
Takeaways
As many parents have said to their newly licensed teenage children, “just because you can drive doesn’t mean you really know how to drive.” The same principle holds here, specifically in the sedation realm, but also regarding dental practice generally. It is, of course, necessary for practitioners to obtain all required credentials in their jurisdictions of practice, but the abilities to perform the range of tasks needed for safe practice do not instantaneously develop on the day a degree or certificate is conferred; rather those abilities will mature with time, so it is the obligation of every practitioner to practice at levels commensurate with their skills at the time, in order to properly protect their patients.
This case study is not meant to promote the specific opinions of the involved Board or its expert, but the study’s purpose is to demonstrate some of the approaches employed in the state’s oversight of its licensed professionals. Unlike courts and juries sitting on dental malpractice cases, in which they must determine whether a plaintiff has demonstrated that negligence has directly caused damages, Boards look simply at the actions of professionals, regardless of the extent or even existence of damages, to determine whether those actions fall within the standards by which their mandates provide.
The process of obtaining pre-treatment medical clearance played a significant role in this case, but that is, by no means, an approach limited to dental treatment under sedation or general anesthesia. Dentists are often confronted with patients suffering from numerous medical conditions, and it is left to those dentists to determine whether it is safe to proceed based upon the information provided by the patient and taking into account their own knowledge and experience, as compared with seeking a medical opinion before going forward. That is a personal determination, always keeping the patient’s best interests in mind. But even when medical clearance is provided by a physician, it is the dentist who bears the ultimate responsibility for the patient’s welfare. So, while a medical clearance is a valuable, and sometimes necessary procedural step, it is best viewed as one of many factors to consider as treatment decisions are made. Perhaps the most important concept from this case is the need for every practitioner to be fully familiar with every drug employed, every potential interaction, every procedure performed, and every realistic side effect. That is precisely what makes a professional. If in doubt, it might well be what is best for the patient to defer or refer.
Note that this case presentation includes circumstances from several different closed cases, in order to demonstrate certain legal and risk management principles, and that identifying facts and personal characteristics were modified to protect identities. The content within is not the original work of MedPro Group but has been published with consent of the author. Nothing contained in this article should be construed as legal, medical, or dental advice. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your personal or business attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
Additional Risk Tips content
Why Accurate Documentation Matters Before Referral and Surgery
In this case study, inaccurate referral information leads to wrong site surgery and a malpractice claim. Read the case to learn how to prevent errors.

How to Stay Passionate in Your Dental Career
Insights on sustaining passion in a dental career through education, community support, work-life balance, and meaningful patient relationships.

Dentist’s Choice of Radiographic Technique Leads to Lawsuit
In this case study, radiographic imaging decisions for a dental implant procedure leads to a malpractice suit. Read the case to learn how the case unfolded.
This document does not constitute legal or medical advice and should not be construed as rules or establishing a standard of care. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
MedPro Group is the marketing name used to refer to the insurance operations of The Medical Protective Company, Princeton Insurance Company, PLICO, Inc. and MedPro RRG Risk Retention Group. All insurance products are underwritten and administered by these and other Berkshire Hathaway affiliates, including National Fire & Marine Insurance Company. Product availability is based upon business and/or regulatory approval and/or may differ among companies.
© MedPro Group Inc. All rights reserved.