Complex Orthodontics Case by a Pediatric Dentist
Case Study
Marc Leffler, DDS, Esq.
January 16, 2025
Reading time: 7 minutes
Background Facts
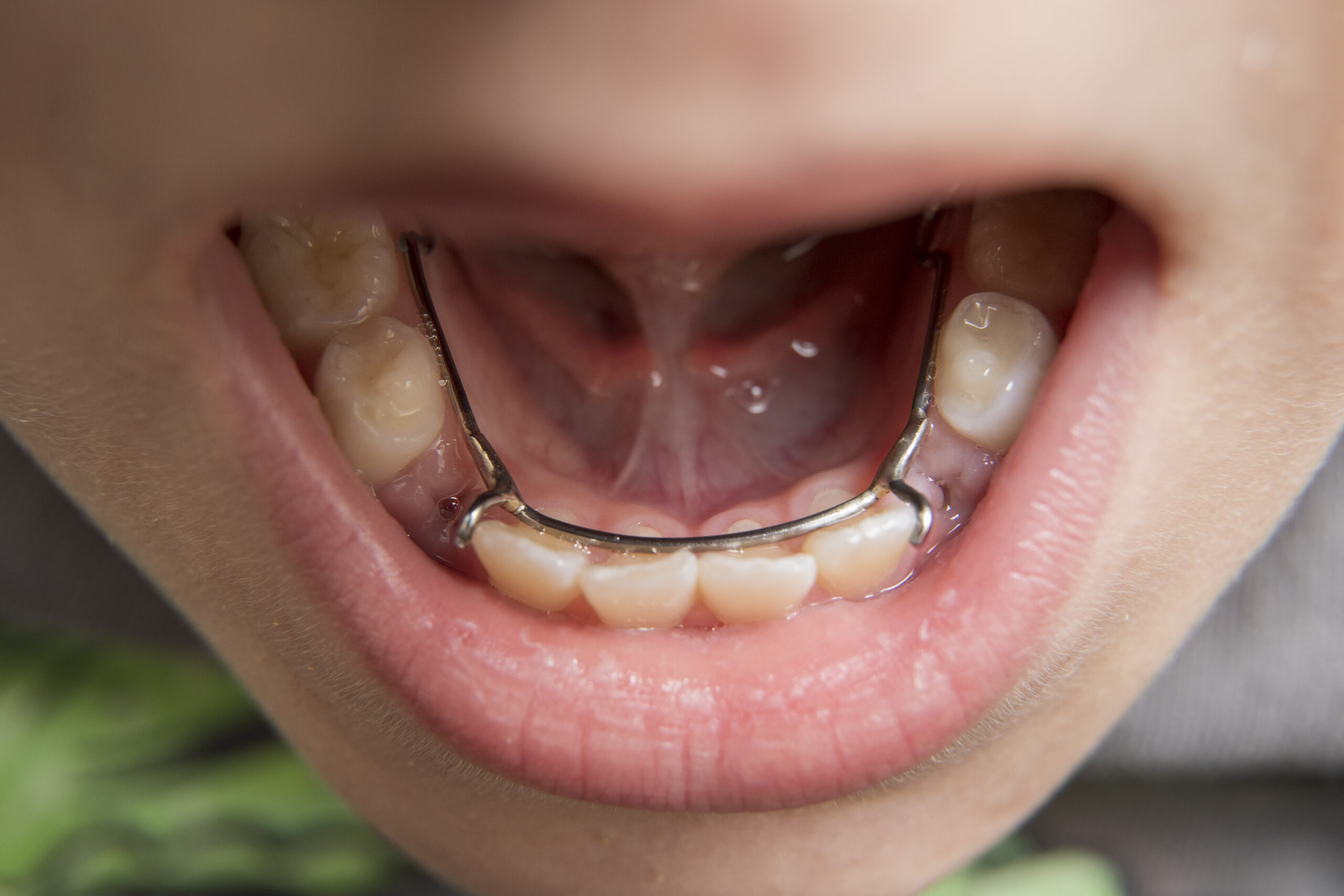
An 11-year-old boy presented with his father to a dental office in which 2 general dentists and a pediatric dentist practiced. The patient and his father met initially with a general dentist (the practice owner) to address the chief complaint of being “unhappy with how the teeth fit together”. On examination, the patient had a bimaxillary protrusion with a mixed dentition. The general dentist saw this as an orthodontics case, so he referred the patient to the pediatric dentist in the office.
The pediatric dentist (we’ll call him Dr. A) had completed his university-based specialty training about 2 years prior, during which he had been involved with 6 orthodontics cases under the supervision of orthodontists. Since going into private practice, he had completed 2 pediatric orthodontics cases and another was close to conclusion. None of those cases included the extraction of any teeth for space-gaining purposes.
Dr. A evaluated the patient clinically, as well as with panoramic and lateral cephalometric radiographs, and study models. He determined that the best treatment was to extract 4 bicuspids and then close the spaces created with full-arch orthodontics. Dr. A met with both parents and their child to discuss the plan, his view as to why the extractions were necessary as compared with realigning the teeth without extractions, the anticipated treatment time of 18-24 months, with retention following, and the fees. After considering for 2 weeks what Dr. A had discussed with them, the parents and the patient agreed to proceed. A written consent form setting all of this out was explained to — and signed by — the patient’s mother.
Dr. A asked the same general dentist (we’ll call him Dr. B) to perform the extractions of the 4 bicuspids, and documented that request clearly in the chart, specifying the reason. The extractions were performed uneventfully. After the initial post-extraction healing period, the patient returned for Dr. A to place upper and lower bands and brackets, and then wires, so that treatment to reduce the anterior proclination and close the now-edentulous bicuspid spaces could begin.
Several months into treatment, the parents received word from their dental insurance carrier that orthodontics was not covered under their plan. So, they asked the practice owner for a fee reduction, but he refused after what was later described as a “contentious discussion”. The parents were so upset that they decided to leave the practice, and took their son to see an orthodontist (we’ll call her Dr. C).
After performing her own work-up, Dr. C advised the parents that the extraction of the 4 teeth was not necessary, that the proclined upper and lower anterior teeth would best be “verticalized” without closing the edentulous spaces, and that the patient now needed to have implants placed into the 4 extraction sites, to be restored with individual crowns.
The parents contacted Dr. A, asking for copies of their son’s records to be sent to Dr. C, explaining what the orthodontist had told them. The office sent a copy to Dr. C, the orthodontist, as requested. However, Dr. A was very upset by the situation, and confronted the practice owner, Dr. B, saying that he felt forced into treating a complex orthodontics case beyond his abilities. This led to Dr. A resigning his position with animus feelings on both sides.
Dr. C completed the orthodontics case while working in tandem with another dentist who placed and restored 4 implants at the sites where the extracted bicuspids had been.
Legal Action
After consulting with and retaining a seasoned dental malpractice attorney, the mother, on behalf of her son, filed a dental malpractice action against Dr. A. As would be expected, the claims in the case were that Dr. A was negligent in treating the case with the 4 extractions, and that he engaged in treatment which was beyond his experience and training.
The damages claims asserted that, due to the patient’s youth and expected lifespan, both the implants and restorations would need to be replaced multiple times over the course of his life. The plaintiff sought monetary damages to pay for the initial implant and restorative treatment, as well as estimates for the future costs, and pain and suffering associated with having lost 4 permanent teeth and emotional distress in connection with the multiple treatments planned for the future.
Discovery
The records of Dr. C, an experienced orthodontist, were obtained and they included clear statements that the extractions of bicuspids were unnecessary because this was not an extraction case. The records of the general dentist who placed and restored the implants, Dr. B, included the costs for that work, plus an estimate of costs over the patient’s estimated lifetime for replacing the implants and restorations on them.
Deposition testimony of the patient and his parents was entirely consistent with the events at Dr. A’s office and with the records of Dr. B and Dr. C. The deposition testimony of Dr. A revealed his limited experience with orthodontics as of the time of treatment, especially with regard to never before handling an extraction case, and also delved into his discussions with the practice owner regarding his having felt pushed into doing treatment beyond his comfort level. Dr. A, a young and introverted man, felt very intimidated by the process and “dreaded” what a courtroom trial experience would be like.
Case Resolution
Dr. A and his attorneys discussed the various ways the case could play out. Dr. A confided that he was losing sleep and professional confidence as the case moved along. His attorneys employed an expert, an orthodontist, who reviewed the records and deposition testimony. The expert believed that Dr. A’s treatment, but more importantly treatment planning, was appropriate, but that Dr. C’s approach would have been an acceptable alternative from the outset as well.
Considering the entire picture, Dr. A requested that attempts be made to try to settle the case before trial, and that took place in the lead-up to trial, leading to settlement.
Takeaways
With tuition amounts for dental school and non-residency specialty training programs as they are, the vast majority of recent graduates have a significant amount of loan debt, so their ability to obtain and maintain employment is more critical than ever. Therefore, pressures by employing dentists upon new dentists to perform procedures beyond their abilities can place these new dentists into positions of feeling that they must perform whatever treatment comes their way (even if beyond their professional abilities) in order to keep their jobs. This may put dentists into an internal battle, pitting ethical responsibilities to “do no harm” against financial obligations. It is a conflict without easy answers, but potentially severe repercussions.
That issue aside, this case raises a repeating theme in dentistry: the unabashed “throwing under the bus” of one dentist by another dentist — a concept referred to as “jousting”. Whether this is done through discussions with patients, in chart entries, by willingness to cooperate with plaintiffs’ attorneys, or all of these, dentists become engaged in this way far more frequently, at least anecdotally, than their colleagues in medicine. Why this happens is a matter of speculation, but the fact that it does leads to lawsuits, disciplinary complaints, and countless time and money spent in defense.
The often-referenced dental school quip of “put 10 dentists in the room and you’ll get 10 different opinions” has changed to “if our opinions differ, I’m right and you’re wrong”, which does not promote advancement of the profession, either among dentists alone or when involving patients. Perhaps elevating discourse in settings such as study clubs, continuing education classes, local dental society meetings, or publications would decrease this growing trend.
Disagreements between patients and dentists – especially about money – are common reasons that patients become plaintiffs. This case demonstrates one such example, namely the incorrect presumption by the parents that the treatment would be covered by insurance. While not always possible, obtaining insurance carrier responses to pre-authorization requests, before treatment is begun, will eliminate unknowns and presumptions in terms of dental costs, reducing the risk of financial disputes.
Related to this is the effect that a refusal on the part of a dentist to reduce fees, or even offer refunds under certain circumstances, can have. In this case, it was that rejected fee reduction request which started the unraveling of the dentist-patient relationship, which in turn led to seeking other care, and ultimately to litigation. It is not the purpose of this writing to advise dentists as to how to handle financial issues with patients, but it is a factor seen often by malpractice defense counsel.
Settlements of dental malpractice cases occur for various reasons. Sometimes, treatment is not able to be defended by experts, making settlement the preferred approach. But even when treatment is defensible, although questionable, pursuing the settlement option may be a matter of a dentist’s desire for resolution, so that practice and personal lives can normalize. Being involved in a lawsuit as a defendant is stressful and time-consuming, so prevention is the best medicine.
Note that this case presentation includes circumstances from several different closed cases, in order to demonstrate certain legal and risk management principles, and that identifying facts and personal characteristics were modified to protect identities. The content within is not the original work of MedPro Group but has been published with consent of the author. Nothing contained in this article should be construed as legal, medical, or dental advice. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your personal or business attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
Additional Risk Tips content
Why Accurate Documentation Matters Before Referral and Surgery
In this case study, inaccurate referral information leads to wrong site surgery and a malpractice claim. Read the case to learn how to prevent errors.

How to Stay Passionate in Your Dental Career
Insights on sustaining passion in a dental career through education, community support, work-life balance, and meaningful patient relationships.

Dentist’s Choice of Radiographic Technique Leads to Lawsuit
In this case study, radiographic imaging decisions for a dental implant procedure leads to a malpractice suit. Read the case to learn how the case unfolded.
This document does not constitute legal or medical advice and should not be construed as rules or establishing a standard of care. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
MedPro Group is the marketing name used to refer to the insurance operations of The Medical Protective Company, Princeton Insurance Company, PLICO, Inc. and MedPro RRG Risk Retention Group. All insurance products are underwritten and administered by these and other Berkshire Hathaway affiliates, including National Fire & Marine Insurance Company. Product availability is based upon business and/or regulatory approval and/or may differ among companies.
© MedPro Group Inc. All rights reserved.