Anterior Endodontic Treatment Leading to Paresthesia
Case Study
Marc Leffler, DDS, Esq.
June 1, 2022
Reading time: 7 minutes
Background Facts
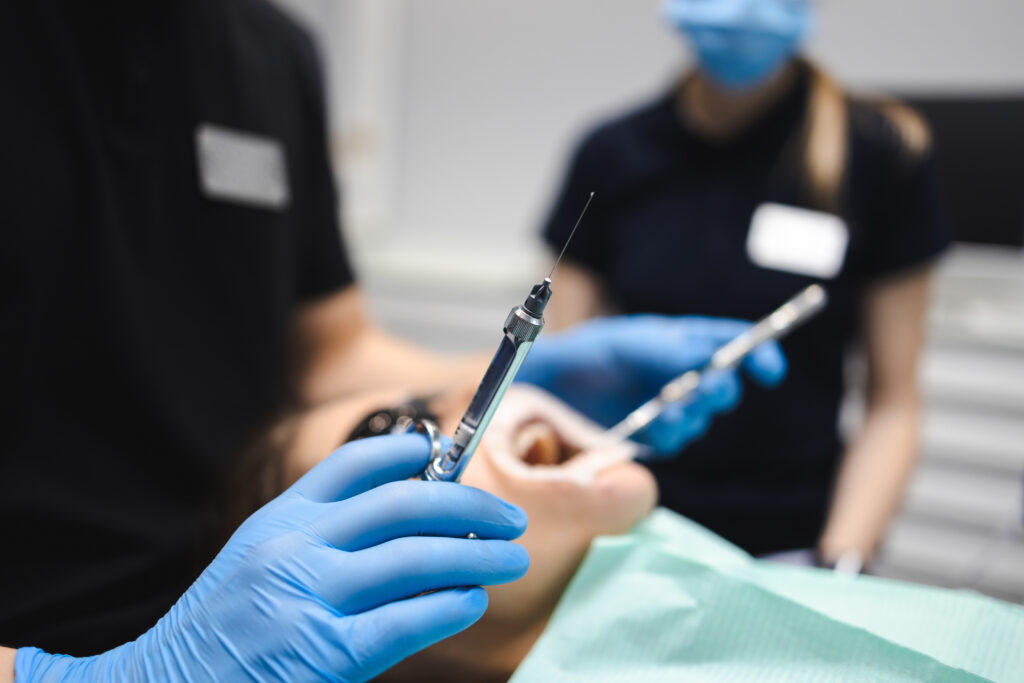
A 37-year-old man presented to his general dentist in excruciating pain associated with a lower left canine tooth, #22; the tooth had undergone trauma during a hockey game years ago, but had been asymptomatic since days after that event. Even though the tooth looked radiographically to require endodontic treatment (RCT) which would be straightforward, the dentist chose to refer the patient to an endodontist due to the patient’s severe symptoms. Within an hour, the patient presented to a local endodontist with a printout of the periapical in hand, but the endodontist took a Panorex as well before doing her examination; it was clear that RCT was needed.
Consent for the procedure was obtained, but with the apex of #22 lying well anterior to the mental foramen, the endodontist did not view or express paresthesia as a real risk. Local infiltration with one carpule of Septocaine (Articaine HCl 4% with epinephrine) was delivered but the symptoms barely abated, so a mandibular block using an additional carpule of the same anesthetic was given, fully anesthetizing the area. The RCT uneventfully went forward to completion, with the final film showing the single canal densely filled to the radiographic apex with gutta percha. The chart entries documented the anesthesia and endodontic procedures in appropriate detail.
At a post-treatment visit two weeks later, the patient asked why “the Novocaine never wore off.” The endodontist suspected that this was a temporary condition, so she re-appointed the patient for two months afterward, at which time the condition was found not to have changed. The endodontist referred the patient to an oral surgeon, who examined the patient and explained to him that he believed the persistent numbness was related to the block injection, so it was not amenable to surgical correction. Normal feeling never returned.
Legal Status
The patient retained an attorney to pursue an action against the endodontist. Records were obtained and a dental malpractice action was filed, claiming negligence but not claiming lack of informed consent, for unknown reasons.
The endodontist notified her malpractice insurance carrier upon being served with papers, and defense attorneys were assigned. By way of the usual exchange between counsel at the early stages of litigation, the claims of negligence were quite specific: improper injection technique and inappropriate use of Septocaine for a mandibular block injection, thereby causing permanent injury to the left inferior alveolar nerve.
Litigation Events
Following the deposition testimony of the patient, now plaintiff, the deposition of the endodontist was scheduled. In preparation, the endodontist and her attorneys met several times, to fully advise her of the process and make sure she knew the types of questions she could reasonably expect. During and outside of these sessions, she reviewed the details of the anatomy and pathways of the inferior alveolar nerve and the other cranial nerves which course the oral cavity, planned her explanation of every detail she used in her block injection technique, which was being criticized as negligent, and reviewed scientific information about Septocaine and the other frequently used local anesthetics.
At deposition, she testified that, although she could not remember giving this particular injection some two years prior, she always used and still uses the same technique every time, which she provided in “textbook” fashion. Questioning about Septocaine was detailed, particularly focusing on a number of published papers which anecdotally described cases of paresthesia following block injections of Septocaine in non-surgical settings; she fully expected this line of questioning and did not provide any testimony counter to her position.
Here, the injury was not a questioned issue, but a viable case of dental malpractice requires that a negligently-performed procedure, as opposed to simply a procedure, be the cause of the injury. So, without any evidence from which the plaintiff’s dental expert could conclude that the injection technique was improper, i.e. negligent, that claim was withdrawn, leaving the only remaining claim that Septocaine should not have been used for a mandibular block injection due to its propensity to function as a neurotoxin and cause nerve injuries.
In the lead-up to trial, defense counsel asked the judge for a Frye Hearing, given the one very limited issue and its nature. In the many states that employ this standard, this type of hearing seeks to establish whether the theory — here, that Septocaine is neurotoxic and, therefore, should not be used for block injections — is one that is “generally accepted in the relevant scientific community”, or, instead, “junk science”, the latter of which is inadmissible. At the Frye Hearing, plaintiff’s expert general dentist argued that Septocaine is a known neurotoxin not to be used for mandibular blocks, with Lidocaine or Carbocaine the proper drugs for that purpose; on cross-examination by defense counsel, the expert was unable to reference any publication which was anything but an anecdotal case report, and he also acknowledged that there had been reported cases of nerve injury following injections with Lidocaine and Carbocaine.
Defense counsel produced a dental school faculty member in the endodontics department who had additional training in biochemistry. This expert testified that formal research studies in refereed journals had debunked the neurotoxicity theory, provided copies of those studies to the court, and explained why, from a biochemical standpoint, neither Septocaine, Lidocaine nor Carbocaine was neurotoxic. The dental community, this expert explained, does not accept the approach of the plaintiff, and has not for some time. The judge concluded that the plaintiff had not demonstrated scientific community acceptance of his theory. With nothing else left in plaintiff’s case, his attorney discontinued the case.
Takeaways
Even though this case did not contain a claim of lack of informed consent, most dental malpractice case filings do have such a claim, and the facts here certainly would have justified it and would have been a challenge for the defense to overcome. With State differences as to specifics, the general proposition regarding informed consent requirements is that a patient must be advised before a procedure of the foreseeable risks, the benefits, and the viable alternatives with their risks. Here, the endodontist specifically excluded the risk of paresthesia due to the distance of the tooth from the mental foramen, but paresthesia does at times occur following mandibular block injections. It raises a question to be considered as to whether giving a block injection for any procedure warrants such a warning; we do not provide an answer, as that choice belongs with the dentist’s judgment, based upon a number of factors associated with a given set of circumstances.
This case contains two situations where referrals were made, the first from the general dentist to the endodontist to perform the procedure, and the second to an oral surgeon when a problem arose. As to whether to perform a procedure or refer the patient, dentists properly base their judgments in this regard upon their own training and experience, and the specific patient circumstances and needs. When complications develop, the assessment is essentially the same, with the added factor of whether the time within which action must be taken for the patient’s well-being is limited. In litigation, dentists are often questioned about whether s/he had an adequate level of skill to have performed a procedure or evaluation, as compared with a dental specialist, so this thought process is always a beneficial one.
The defense attorneys’ preparation of the endodontist for deposition proved valuable and case-changing by focusing their client into the relevant areas of planning. Similarly, the endodontist became thoroughly acquainted with all of the case subject matters in order to best be able to advocate for herself; she did a review of research and re-familiarized herself with anatomy. Litigation is a team effort between client, attorney, expert witnesses, and insurance company.
Problems do sometimes occur following dental treatment, but that does not necessarily equate to malpractice. Good records which document events and findings are, perhaps, the most valuable tool for defense attorneys.
Finally, the use of a less-than-common pre-trial technique, the Frye Hearing, proved dispositive. It is not expected that dentists would be at all familiar with it, but it demonstrates how an insurance carrier and its experienced defense attorneys can team up for a successful result.
Note that this case presentation includes circumstances from several different closed cases, in order to demonstrate certain legal and risk management principles, and that identifying facts and personal characteristics were modified to protect identities. The content within is not the original work of MedPro Group but has been published with consent of the author. Nothing contained in this article should be construed as legal, medical, or dental advice. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your personal or business attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
Additional Claims content

Understanding Dental Malpractice Cases: Answers to Common Questions
Claims
The average dentist gets sued at least once in their career, and it’s important for dentists to be prepared in the event they must face a lawsuit. In this article, we’ll answer eight common questions about malpractice claims and lawsuits.
Communication Mishap Between Providers Leads to Malpractice Suit
Claims
Proper communication between dental providers is essential when referring a patient for a procedure. In this case study, a dentist refers a patient to an oral surgeon for a tooth extraction, but a miscommunication between the providers causes the oral surgeon to extract the wrong tooth.

Loss of Taste After Procedure Leads to Lawsuit Against Dentist
Claims
Informed consent is one of the most important aspects of dental care. When performing a procedure, ensuring through verbal agreement and documentation that a patient understands all possible negative outcomes is the best way to protect yourself against claims of negligence and malpractice lawsuits. In this case study, a dentist’s informed consent documentation becomes key when she is sued over a patient’s loss of taste after a procedure.
This document does not constitute legal or medical advice and should not be construed as rules or establishing a standard of care. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
MedPro Group is the marketing name used to refer to the insurance operations of The Medical Protective Company, Princeton Insurance Company, PLICO, Inc. and MedPro RRG Risk Retention Group. All insurance products are underwritten and administered by these and other Berkshire Hathaway affiliates, including National Fire & Marine Insurance Company. Product availability is based upon business and/or regulatory approval and/or may differ among companies.
© MedPro Group Inc. All rights reserved.